Sclerotherapy FAQ
What is sclerotherapy?
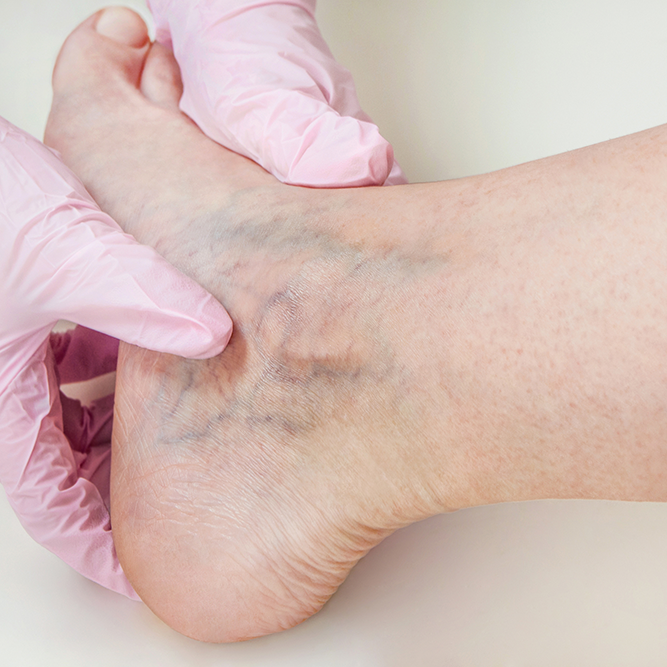
Sclerotherapy is a popular method of eliminating varicose veins and superficial telangioectasis (spider veins) in which a solution, called a sclerosing agent, is injected into the veins.
Does sclerotherapy work for everyone?
The majority of persons who have sclerotherapy performed will be cleared of their varicosities or at least see good improvement. Unfortunately, however, there is no guarantee that sclerotherapy will be effective in every case. Approximately 10% of patients who undergo sclerotherapy have poor to fair results. (“Poor results” means that the veins have not totally disappeared after six treatments.) In very rare instances, the patient’s condition may become worse after sclerotherapy treatment.
How many treatments will I need?
The number of treatments needed to clear or improve the condition differs from patient to patient, depending on the extent of varicose and spider veins present. One to six or more treatments may be needed; the average is three to four. Individual veins usually require one to three treatments.
What are the most common side effects of sclerotherapy?
The most common side effects experienced with sclerotherapy treatments are
- 1. ITCHING – Depending upon the type of solution used, you may experience mild itching along the vein route. This itching normally lasts 1 to 2 days.
- 2. TRANSIENT HYPERPIGMENTATION – Approximately 30% of patients who undergo sclerotherapy notice a discoloration of light brown streaks after treatment. In almost every patient, the veins become darker almost immediately after the procedure. In rare instances, this darkening of the vein may persist for 4 to 12 months.
- 3. PERMANENT HYPERPIGMENTATION – A permanent discoloration (usually small and hardly noticeable but which may be objectionable from a cosmetic viewpoint) may remain along the path of the sclerosed segment.
- 4. SLOUGHING – Sloughing occurs in less than 3% of patients who receive sclerotherapy. Sloughing consists of a small ulceration at the injection site that heals slowly. A blister may form and then may open and become ulcerated. The scar that follows should return to a normal color.
- 5. ALLERGIC REACTION – Very rarely, a patient may have an allergic reaction to the sclerosing agent used. The risk of an allergic reaction is greater in patients who have a history of allergies.
- 6. PAIN – A few patients may experience moderate to severe pain and some bruising, usually at the site of the injection. The veins may be tender to the touch after treatment and an uncomfortable sensation may run along the vein route. This pain is usually temporary, in most cases lasting 1 to 7 days, at the very most.
What are the other side effects of sclerotherapy?
Other, less common, side effects include a burning sensation during injection of some solutions, neovascularization (the development, usually temporary, of new, tiny blood vessels), transient phlebitis-type reactions (swelling of the vein) which might cause the ankles to swell, temporary superficial blebs or wheals (similar to hives), and, very rarely, wound infections, poor healing, or scarring.
Rare complications of sclerotherapy include visual disturbances and transient ischaemic attacks or stroke.
How likely is phlebitis to occur following sclerotherapy?
Phlebitis is a very rare complication, seen in approximately one out of every 1000 patients treated for varicose veins which are greater than 3 to 4 mm. in diameter.
What are the dangers of phlebitis?
The dangers of phlebitis include the possibility of pulmonary embolus (a blood clot to the lungs) which may result in permanent lung damage or death, and post-phlebitis syndrome, in which the blood clot is not carried out of the lungs, resulting in permanent swelling of the legs.
What are possible complications of varicose veins if I do not have sclerotherapy?
In most cases of large varicose veins (greater than 3 to 4 mm. in diameter), spontaneous phlebitis and/or thrombosis (blood clot) may occur. Additionally, large skin ulcerations may develop in the ankle region of patients who have long-standing varicose veins with underlying venous insufficiency. Rarely, those ulcers may hemorrhage or become cancerous.
Are there other types of procedures to treat varicose veins and telangiectasias?
VNUS Closure may also be used to treat varicose veins, but not telangiectasias. The VNSU Closure procedure requires outpatient surgery and is performed while the patient is under local anesthesia and sedation. This type of surgery is usually reserved for patients with large varicose veins not amenable to sclerotherapy or patients with significant incompetence of their greater saphenous vein. Sometimes a combination of surgery and sclerotherapy is required.
What if I experience a problem after receiving sclerotherapy?
If you notice any type of adverse reaction, please call our office immediately: 617.244.5355.
What are the medical billing codes for sclerotherapy?
- Sclerotherapy Code #36471 for varicose veins
- Sclerotherapy Code #36468 for spider veins (this is almost never a service covered by insurance)
Boston SansVein & Esthétiques: An IAC accredited vein center, where our expert vascular surgeon, Dr. Sentissi, and her team can evaluate and treat your veins – from spider veins to varicose veins – and get you looking and feeling great.

Dr. Sentissi performed a veinous closure on one leg and will be doing the same for my other leg shortly. She is extremely professional, efficient, and personable. I was very comforted by her demeanor and felt certain the outcome would be positive, which it has been. There was virtually no pain after the procedure and everything that Dr. Sentissi stated to expect, happened almost like clockwork. She also has a highly competent staff, including Brenda and Lauren.
From the start she put me at ease; was extremely knowledgable, patient, answered all my questions, and made me not dread the surgery at all. I could tell I was in very good hands.
Dr. Sentissi is wonderful! Very professional and very courteous. My procedure was 100% successful. In addition, the assistants and office staff are very helpful and responsive to questions. I highly recommend Dr. Sentissi and the entire office!
